Joint Pain
Biological Mechanisms, Causes, and Therapeutic Approaches
Joint pain, clinically referred to as arthralgia, is a common symptom in medical practice and may result from multiple pathophysiological processes, including inflammation, cartilage degeneration, metabolic alterations, and immune system dysfunction.
Joints are highly specialized biomechanical structures responsible for enabling mobility and distributing mechanical loads throughout the musculoskeletal system. Any alteration affecting their structural components—such as cartilage, synovial membrane, ligaments, or subchondral bone—can trigger inflammatory or degenerative processes that lead to pain and functional limitation.
The following sections examine the primary biological mechanisms involved in joint pain.
1. Joint Structure and Physiology of Articular Pain
Synovial joints are complex anatomical systems composed of several structural and biochemical elements that work together to facilitate smooth movement and mechanical load distribution.
Key components include:
Articular Cartilage
Articular cartilage is a specialized form of hyaline cartilage that covers the ends of bones within a joint. Its primary function is to reduce friction and absorb mechanical shock during movement.
The extracellular matrix of cartilage is mainly composed of:
Type II collagen
Proteoglycans (especially aggrecan)
Water, which can represent up to 80% of the tissue
Cartilage is avascular, meaning it does not have a direct blood supply. Instead, its nutrients are supplied through diffusion from the synovial fluid.
Synovial Membrane
The synovial membrane lines the inner surface of the joint capsule and is responsible for producing synovial fluid, a viscous fluid rich in hyaluronic acid that functions as a biological lubricant.
Inflammatory changes in the synovial membrane can significantly alter joint physiology by increasing the production of inflammatory cytokines such as:
IL-1β
TNF-α
IL-6
These cytokines stimulate cartilage degradation and activate nociceptive pathways responsible for pain perception.
Subchondral Bone
Subchondral bone is the layer of bone located directly beneath the articular cartilage. It plays a critical role in absorbing mechanical stress and maintaining joint stability.
Structural alterations in this bone layer can increase mechanical stress on cartilage and contribute to degenerative joint disease.
Mechanism of Pain Generation
Importantly, cartilage itself does not contain nerve endings. Therefore, articular pain originates primarily from nociceptors located in:
the synovial membrane
the joint capsule
ligaments
the subchondral bone
Inflammatory processes increase the release of mediators such as:
prostaglandins
bradykinin
inflammatory cytokines
These molecules lower the activation threshold of nociceptive nerve fibers, resulting in increased pain sensitivity.
2. Major Diseases Associated with Joint Pain
Several pathological conditions can affect joint structures. Among the most clinically relevant are degenerative, autoimmune, and metabolic disorders.
Degenerative Joint Diseases
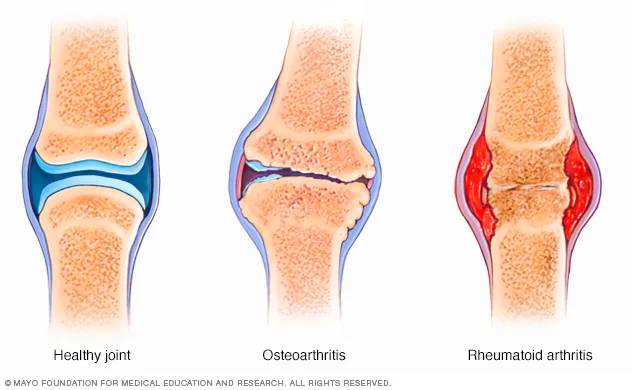
Osteoarthritis is the most common chronic joint disorder worldwide.
It is characterized by a progressive degeneration of articular cartilage accompanied by structural changes in surrounding tissues.
Key pathological features include:
progressive cartilage breakdown
remodeling of subchondral bone
formation of osteophytes (bone spurs)
mild synovial inflammation
At the molecular level, increased activity of degradative enzymes such as:
matrix metalloproteinases (MMP-1, MMP-13)
aggrecanases
leads to breakdown of cartilage extracellular matrix components.
This degradation reduces the joint’s ability to absorb mechanical forces, resulting in pain and stiffness.
Autoimmune Disorders
Rheumatoid Arthritis is a chronic systemic autoimmune disease primarily affecting synovial joints.
In this condition, the immune system produces autoantibodies, including:
rheumatoid factor (RF)
anti-cyclic citrullinated peptide antibodies (anti-CCP)
These antibodies trigger an intense inflammatory response within the synovial membrane.
The inflammatory process leads to the formation of pannus, an abnormal proliferative synovial tissue that invades and destroys cartilage and bone.
Key immune mechanisms include activation of:
macrophages
T lymphocytes
pro-inflammatory cytokines
Without proper treatment, the disease can lead to irreversible joint deformities and severe functional impairment.
Metabolic Joint Disorders
Gout is an inflammatory arthritis caused by the deposition of monosodium urate crystals within joint tissues.
This condition occurs when serum uric acid levels become persistently elevated, a state known as hyperuricemia.
The urate crystals are recognized by the immune system as foreign particles, activating the NLRP3 inflammasome, which stimulates the release of interleukin-1β (IL-1β) and triggers an acute inflammatory response.
Clinically, gout attacks are characterized by:
sudden onset of severe pain
redness and swelling
warmth in the affected joint
The first metatarsophalangeal joint (the base of the big toe) is the most frequently affected site.
3. The Role of Systemic Inflammation and Metabolism
Recent research has highlighted the important relationship between metabolic health and joint disorders.
A key concept in this field is chronic low-grade systemic inflammation, which is frequently associated with metabolic conditions such as:
obesity
metabolic syndrome
insulin resistance
type 2 diabetes
Adipose tissue, particularly visceral fat, functions as an endocrine organ and releases signaling molecules known as adipokines, including:
leptin
resistin
TNF-α
IL-6
These molecules can amplify inflammatory signaling pathways throughout the body, including within joint tissues.
In addition, chronically elevated blood glucose levels promote the formation of advanced glycation end products (AGEs).
AGEs alter the structural integrity of collagen and other connective tissue proteins, contributing to stiffness, reduced elasticity, and degeneration of joint structures.
4. Therapeutic Strategies and Prevention
Management of joint pain depends on the underlying etiology but typically involves a combination of pharmacological treatment and lifestyle interventions.
Pharmacological Therapies
Common medical treatments include:
nonsteroidal anti-inflammatory drugs (NSAIDs)
corticosteroids
disease-modifying antirheumatic drugs (DMARDs) in autoimmune conditions
biologic therapies targeting inflammatory cytokines
These medications aim to reduce inflammation, alleviate symptoms, and slow disease progression.
Nutritional Interventions
Certain nutrients have demonstrated anti-inflammatory properties that may support joint health.
Examples include:
omega-3 fatty acids
curcumin
polyphenols
vitamin D
These compounds may modulate inflammatory pathways and reduce the production of pro-inflammatory cytokines.
Physical Activity
Regular physical activity plays a critical role in maintaining joint health.
Exercise contributes to:
strengthening periarticular muscles
improving joint stability
enhancing synovial fluid circulation
reducing systemic inflammation
Low-impact activities such as walking, swimming, and resistance training are often recommended.
Conclusion
Joint pain is a complex clinical condition involving interactions between biomechanical stress, immune activity, and metabolic factors.
Understanding these mechanisms is essential for developing effective therapeutic strategies.
Optimal management typically requires a multidisciplinary approach that combines early diagnosis, inflammation control, and lifestyle modification to preserve long-term joint function.
Sources and Further Reading
- [1] The most common types are osteoarthritis and rheumatoid arthritis. Mayo Clinic
- [2] Mayo Clinic Guide to Arthritis Mayo Clinic Guide Book
This is an independent review page. Please note that the information we provide is not intended to replace consultation with a qualified medical professional. We encourage you to inform your physician of changes you make to your lifestyle and discuss these with him or her. For questions or concerns about any medical conditions you may have, please contact your doctor.
Statements on this website have not been evaluated by the Food and Drug Administration. Products are not intended to diagnose, treat, cure or prevent any disease. If you are pregnant, nursing, taking medication, or have a medical condition, consult your physician before using our products.
The website’s content and the product for sale is based upon the author’s opinion and is provided solely on an “AS IS” and “AS AVAILABLE” basis. You should do your own research and confirm the information with other sources when searching for information regarding health issues and always review the information carefully with your professional health care provider before using any of the protocols presented on this website and/or the product sold here.